Dry Eyes After Botox – How to Support Your Patient
Posted on: April 24, 2026
Posted on:
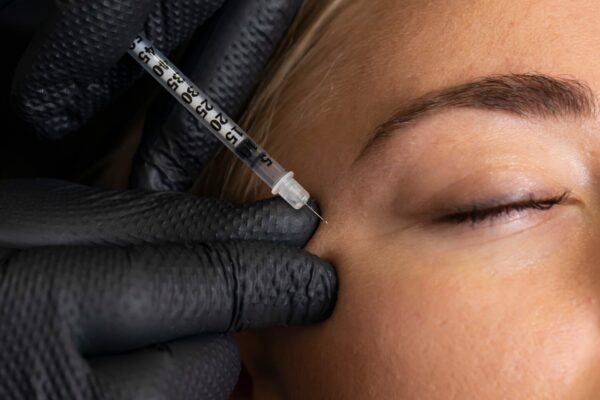
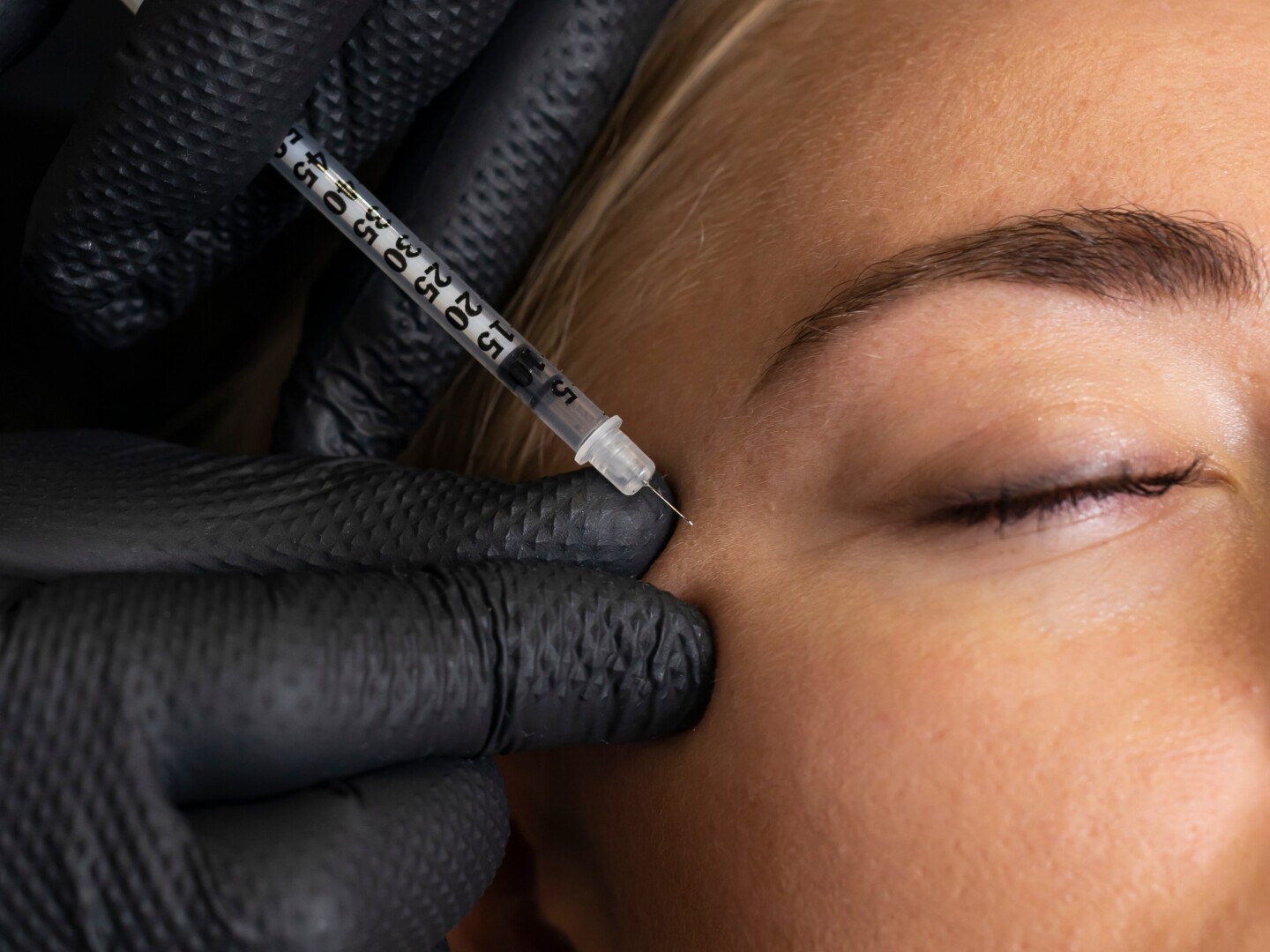
Botulinum toxin, commonly known as Botox or BTX, is a popular treatment in facial aesthetics thanks to its ability to smooth wrinkles and enhance facial balance. It is generally safe, however, injections around the eyes can occasionally lead to dry eyes, which can affect patient satisfaction if the discomfort isn’t managed properly.
For clinicians, it’s important to understand why dry eyes occur, how to recognise early symptoms, and how to support patients. This guide outlines the risk factors, assessment strategies, and steps you can take to ensure safe, comfortable outcomes for everyone receiving Botulinum toxin treatments.
Can Botox cause dry eyes?
Botulinum toxin injections around the eyes can sometimes interfere with eyelid function and tear distribution, which can lead to dry eyes. This is because relaxation of the orbicularis oculi muscle can prevent the eyelids from closing fully, which can reduce the spread of tears across the surface of the eye. Plus, a decreased blink rate can limit they eye’s natural lubrication, and in some cases, nearby glands responsible for tear production can be affected.
Below are some of the symptoms to watch out for in your patients:
- A gritty or burning sensation in the eyes
- Redness or mild irritation
- Excessive tearing as a reflex to dryness
- Sensitivity to light or blurred vision
Risk factors and patient considerations
Not all patients are equally susceptible to developing dry eyes after Botox, so it’s essential to conduct a thorough pre-treatment assessment. Patients who have a history of chronic dry eye, blepharitis, meibomian gland dysfunction, or other ocular surface conditions are at higher risk, as their tear film is already compromised. Similarly, any patient taking medications that are known to reduce tear production, such as antihistamines, certain antidepressants, or isotretinoin, could be more prone to dry eyes after treatment.
Patients who have previously had ocular surgeries or eyelid procedures can also be at higher risk, as these can affect eyelid function and tear distribution. Age is another consideration, as older patients often have naturally reduced tear production and can experience more noticeable symptoms.
The dosage and injection sites around the eyes are critical factors. Higher doses or injections placed too close to the lower eyelid or lateral canthus can weaken the orbicularis oculi muscle, which increases the likelihood of the eyelid not closing fully and decreased blinking. Careful placement, conservative dosing, and awareness of each patient’s anatomical variations can help to reduce the risk of dry eyes.
Finally, it’s important to set realistic expectations during the consultation. Patients should be informed about the possibility of temporary dryness, signs to watch for, and what they can do to stay comfortable.
How to identify and assess dry eye in Botox patients
Early recognition of dry eyes after Botox can be essential to preventing discomfort and potential complications. During consultations, you should ask your patient about any history of eye irritation, dryness, or sensitivity, as well as any recent changes in vision or tear production.
You can quickly perform basic assessment techniques in the clinic. For example, you can ask the patient to blink naturally and observe how the eyelid closes – this can reveal incomplete blinking.
It is also important to monitor your patients post-treatment, especially within the first week, as this is when symptoms often appear. Taking early intervention, such as recommending lubricating eye drops, warm compresses, or adjustments to eyelid function, can significantly improve your patient’s comfort.
If symptoms persist, worsen, or if there is any sign of corneal irritation or damage, you should refer your patient to a specialist.
How to support patients suffering with dry eyes after Botox treatment
If you have identified dry eyes in your patient, or if you anticipate your patient is at high risk, there are a number of steps you can take to support your patient and help keep them comfortable.
Lubricating eye drops or artificial tears are often the first line of defence, as these help to supplement natural tear production and relieve irritation. You can also recommend specific ointments to use at night to keep the eyes hydrated while they sleep.
Lifestyle and environmental adjustments can also make a significant difference. You can suggest your patient takes regular screen breaks, keeps hydrated, and even use a humidifier in dry environments to help reduce their symptoms. Wearing protective eyewear, such as wraparound glasses, can shield the eyes from wind or dust, which can exacerbate dryness.
Eyelid care is another important consideration. Your patient might benefit from warm compresses or gentle eyelid massages to stimulate the natural gland function. In some cases, you might want to consider adjusting the BTX dose or placement in future treatments to reduce the likelihood of ongoing dryness.
Clear communication is vital. You can provide your patients with written aftercare instructions, advising them on what symptoms to monitor, and scheduling follow-up appointments to ensure that any issues are addressed promptly.
Take your botulinum toxin skills further
Whether you’re just starting out or looking to refine your technique, Dr Bob Khanna Training Institute offers a full range of botulinum toxin courses to suit your needs. If you’re new to medical aesthetics, you can gain confidence and essential skills with our Botox courses for beginners. For experienced practitioners, our advanced aesthetics training courses cover the latest techniques and nuanced approaches to achieve optimal results.
Explore our courses today and ensure you can support your patients safely and professionally whilst advancing your expertise in facial aesthetics.